If a picture is worth a thousand words, could it be argued that a video is worth a thousand pictures? More? It’s futile to come up with an equation to measure the impact of motion vs. static medical images, but in my experience as an orthopedic surgeon, one thing has proven clear: there are certain use cases where the ability to see motion is uniquely valuable.
In orthopedic care, seeing anatomy in motion can reveal injuries, instabilities, and conditions that are hard to discern with static images. In this article, I’ll focus on a newer approach to medical imaging – Dynamic Digital Radiography, or DDR – that captures digital motion X-ray images, and I’ll offer examples of specific use cases where I prefer to use DDR over static radiography.
Introducing DDR & Its Benefits
Dynamic Digital Radiography (DDR) is a powerful imaging technology that captures a series of high-quality X-ray images in sequence, creating a dynamic, motion playback view of anatomical motion. DDR compiles a series of images into a “cine loop“; this approach reveals unique insights into function and stability that can only be gleaned from seeing motion.
And because DDR captures frames as intermittent, diagnostic-quality X-ray “pulses” and then strings them into motion, DDR X-rays show enhanced details without requiring as rapid of continuous radiation exposure as traditional fluoroscopy would.
Use Cases for DDR
Dynamic Digital Radiography is uniquely valuable in several clinical scenarios where imaging motion improves diagnosis and treatment planning. These scenarios can be organized into three broad categories: dynamic motion assessments, injury detection and diagnosis, and post-surgical evaluations.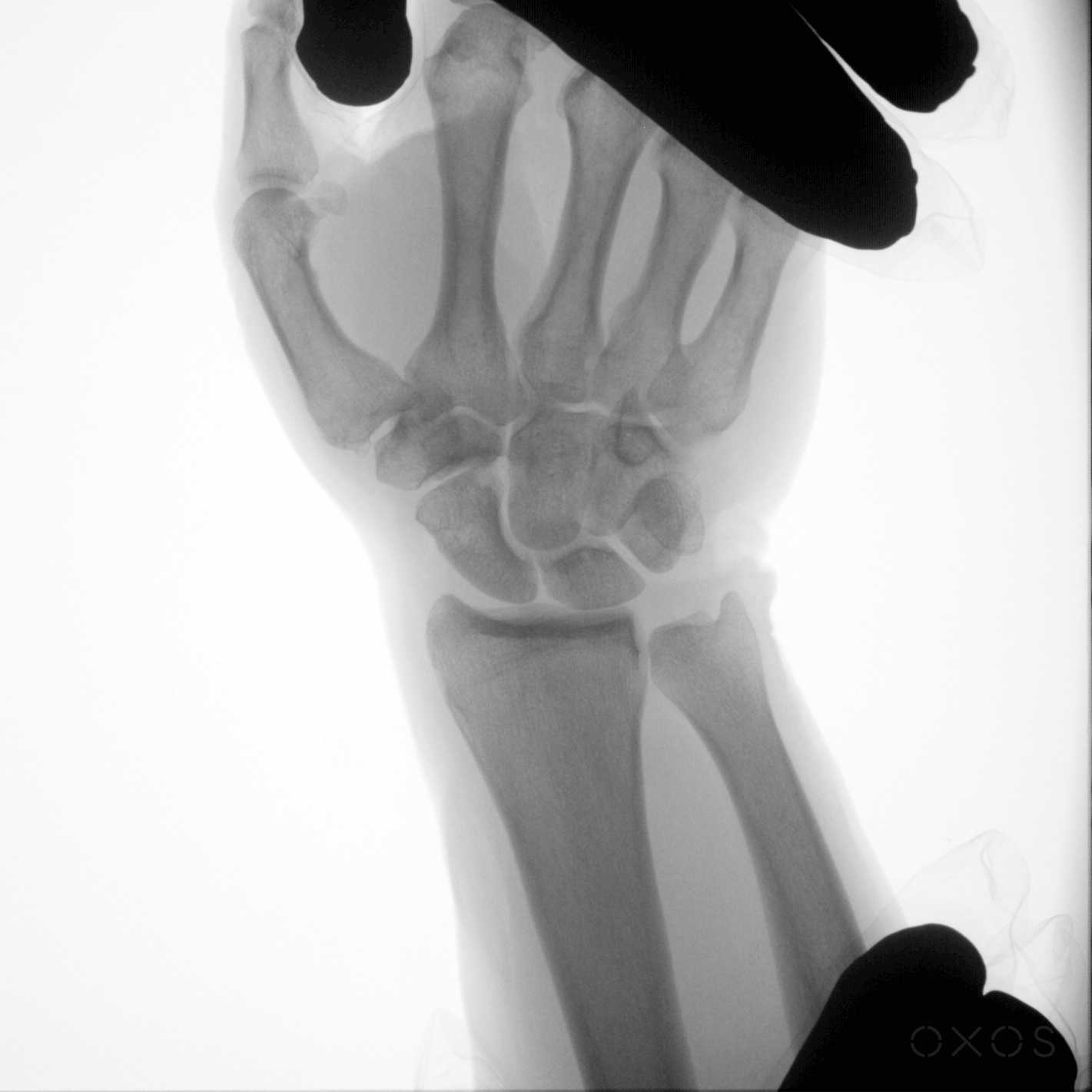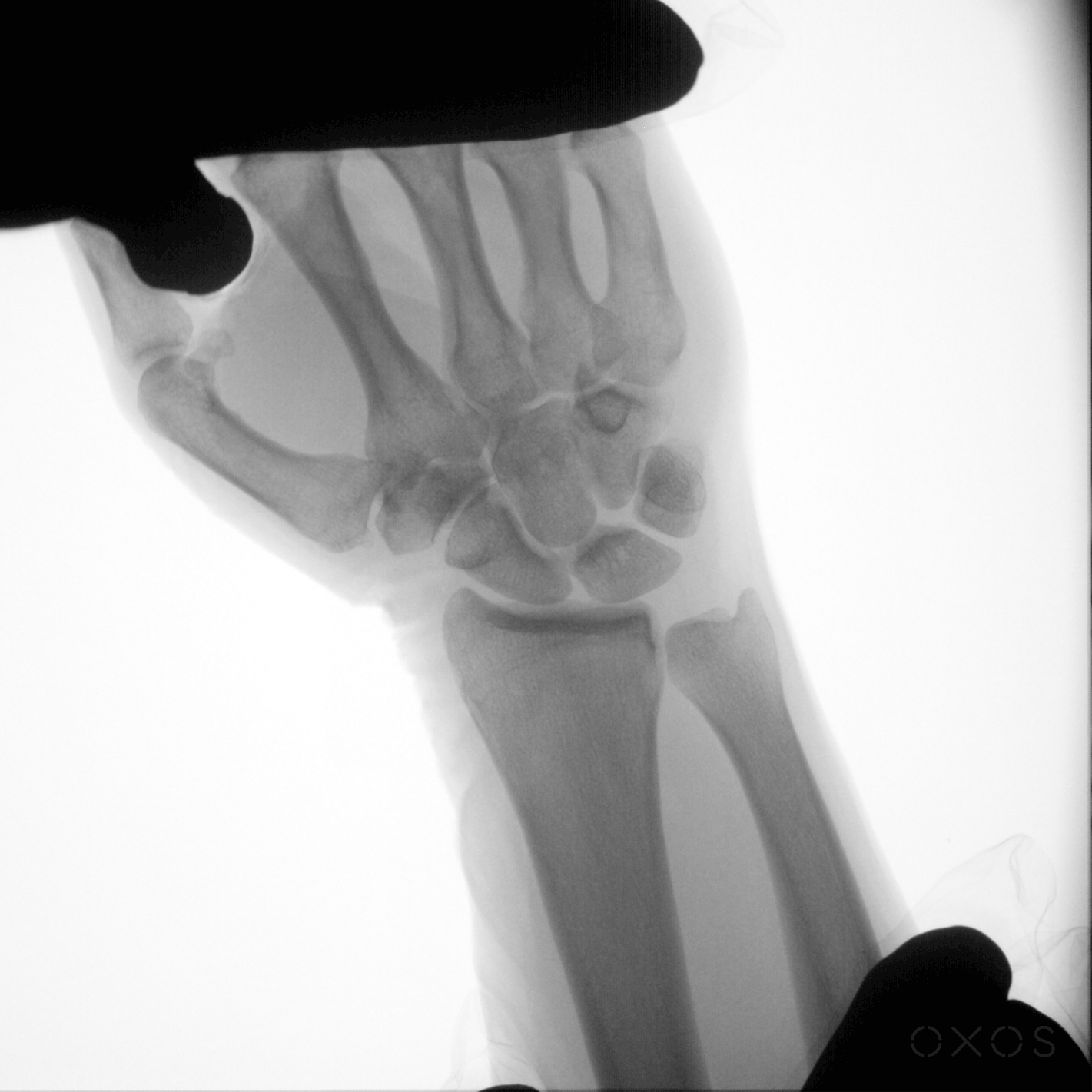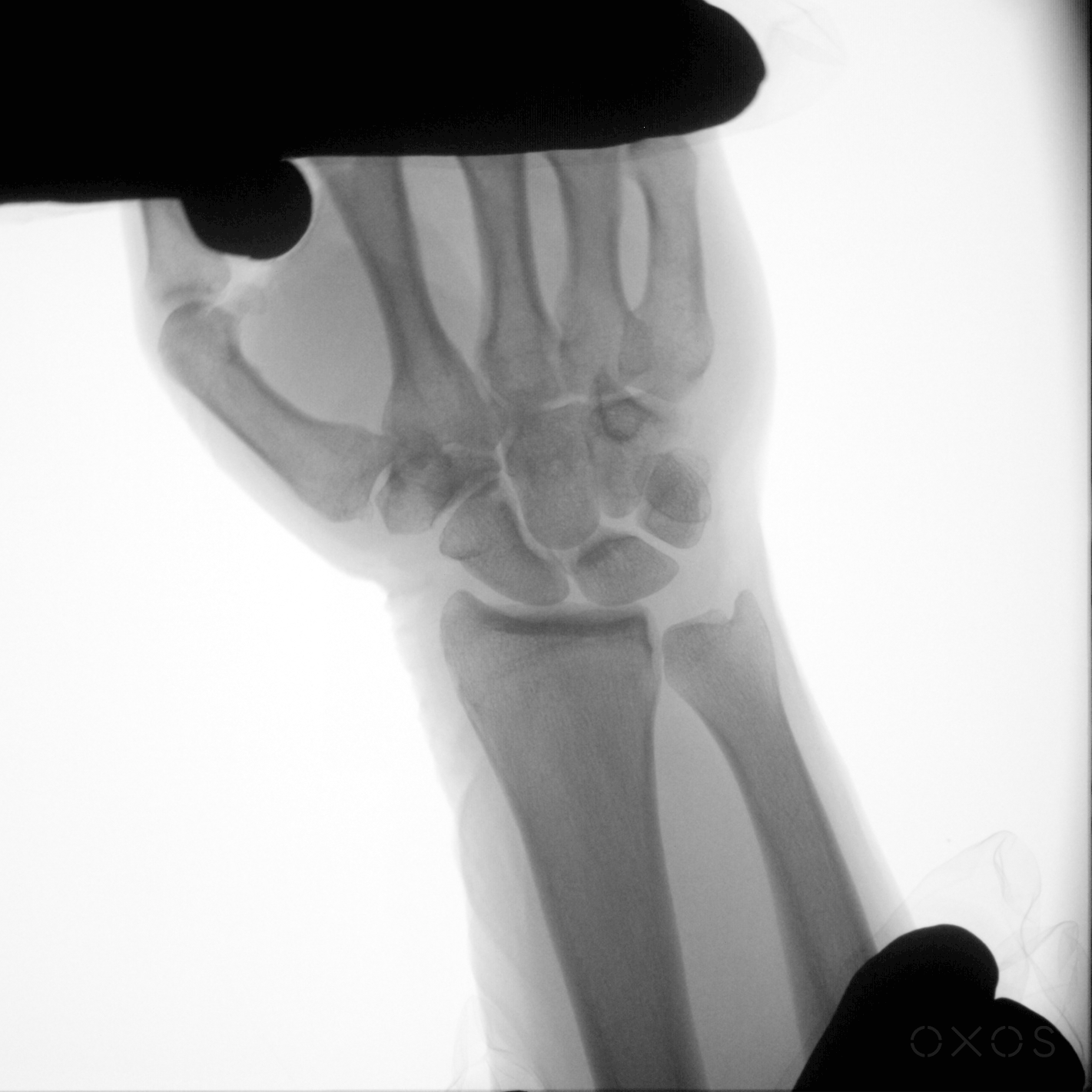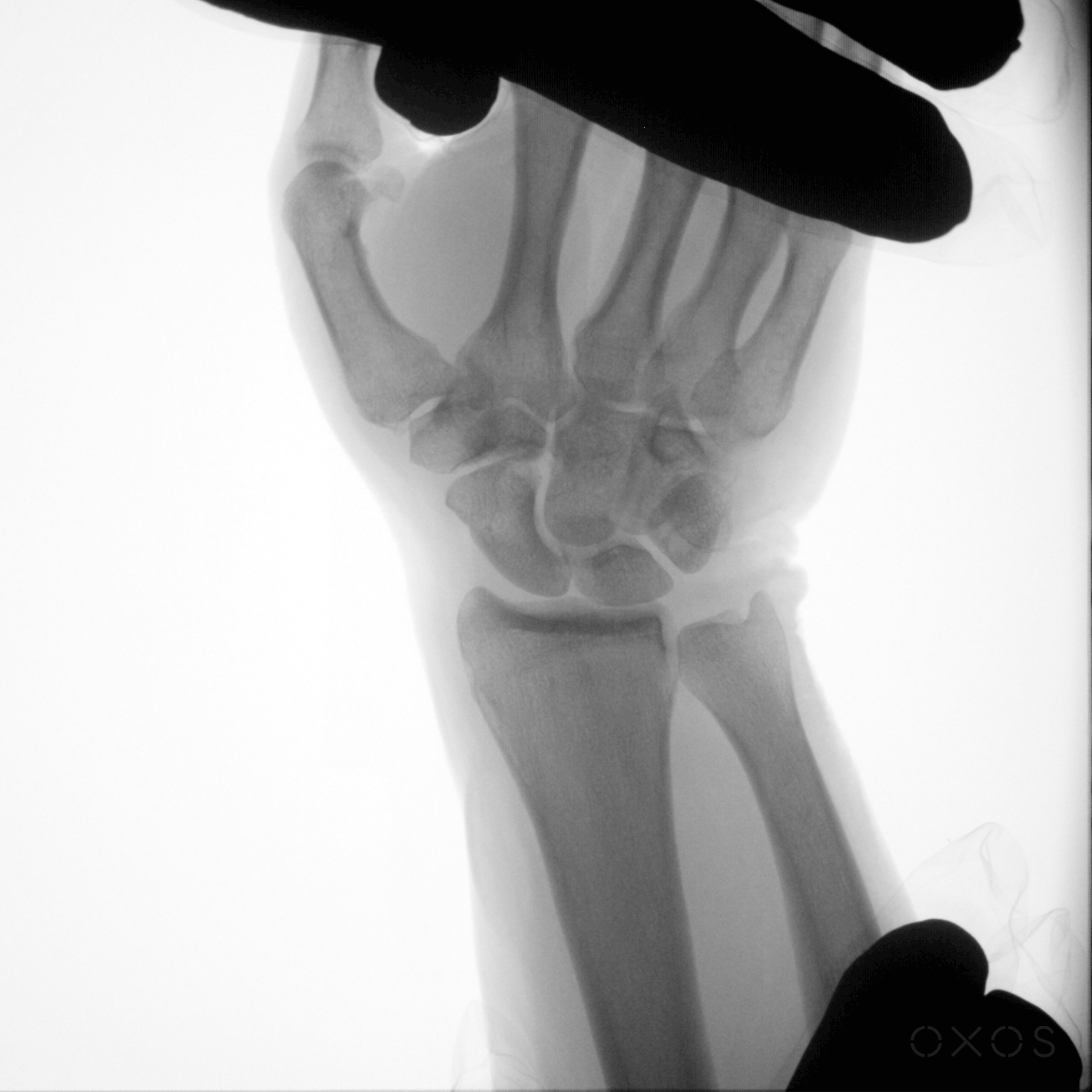
Dynamic Motion Assessment
If the goal is to show functional behavior through motion X-ray, I’ve found DDR to be an optimal mode of medical imaging. Here are some use cases that fall under this category.
- Stress testing ligaments to assess laxity: DDR allows orthopedic surgeons to stress joints while imaging them dynamically, evaluating laxity and subtle instability that would not be visible in static views.
- Visualizing and assessing joint dislocations, relocations, and instability: Dislocation management typically requires multiple static X-rays before and after reductions. With DDR, I can view dislocation and relocation in motion with minimal radiation exposure.
Example: When treating an elbow dislocation or relocation, an X-ray device with DDR capabilities can capture the extension movement dynamically, allowing me to monitor the radiocapitellar and ulnohumeral joints after splinting to make sure they’re stabilized without overextension. - Pre- and post-surgical motion studies: Comparing range of motion before and after surgery is more accurate and revealing with dynamic imaging, helping track surgical success and rehabilitation progress.
Injury Detection and Diagnosis
Diagnosing injuries – especially those that require movement to see abnormalities – can be dramatically simplified with DDR-enabled X-ray technology.
- Identifying ligament tears and syndesmotic injuries: Some injuries — such as AC joint separations in the shoulder or syndesmotic sprains — are easily missed on static X-rays but become obvious with dynamic stress imaging.
Example: DDR allows orthopedic surgeons to dynamically type AC joint injuries by capturing the clavicle’s relationship to the acromion during motion, providing a more accurate diagnosis. - Dislocations and reductions: Imaging during dislocation events allows for more confident reductions and helps avoid missing subtle subluxations or instability.
Post-Surgical Evaluation
Evaluating surgical outcomes and pinpointing ongoing issues before they snowball is another category of X-ray where I’ve found DDR to be beneficial.
- Assessing hardware placement and sources of post-surgical discomfort: DDR helps me observe how implants interact with moving joints, detecting hardware malalignment or issues that might not be evident in static images.
Example: After fixation, patients often struggle with foot/ankle pain. Dynamic evaluation with DDR can isolate sources of pain related to plate or screw placement, helping guide next steps in treatment.
See How DDR Can Benefit Your Patients — and Your Practice
Dynamic Digital Radiography is changing how I capture, diagnose, and treat musculoskeletal injuries. I would encourage other orthopedic surgeons to explore DDR as an innovative new approach to medical imaging.
My own experience with X-ray was one factor that led me to start OXOS Medical, where we’ve incorporated DDR as one of four imaging modes offered in our portable devices. (The other three modes are photography, single radiography, and fluoroscopy.)
A key differentiator of MC2 is its ability to capture high-resolution DDR sequences wherever care is delivered. By combining mobility with the superior image quality of DDR, MC2 empowers orthopedic surgeons to make more accurate, informed decisions at the point of care. I’ve used the Micro C and MC2 in my practice and can validate these claims firsthand.
MC2’s one-hand or hands-free operation also supports joint manipulation and dynamic assessment with anatomical support.
With the MC2 portable X-ray system, orthopedic surgeons can bring high-quality dynamic imaging directly to patients, wherever they are.
I’d encourage other clinicians to experience the difference DDR can make.
Learn more about MC2 here.